Home » Archives for THS Hospital » Page 6
Home » Archives for THS Hospital » Page 6
Sciatica Treatment
S
ciatica is a painful condition caused by a trapped nerve in the spine. The pain typcially starts from the lower back and refers down into the leg. This may be associated with pins and needles, numbness or weakness. Treatment can include physiotherapy, medications, spinal injections, laser spine surgery, keyhole spine surgery or sometimes spinal ozone therapy.
Sciatica can be one of the most painful conditions to affect a persons health.
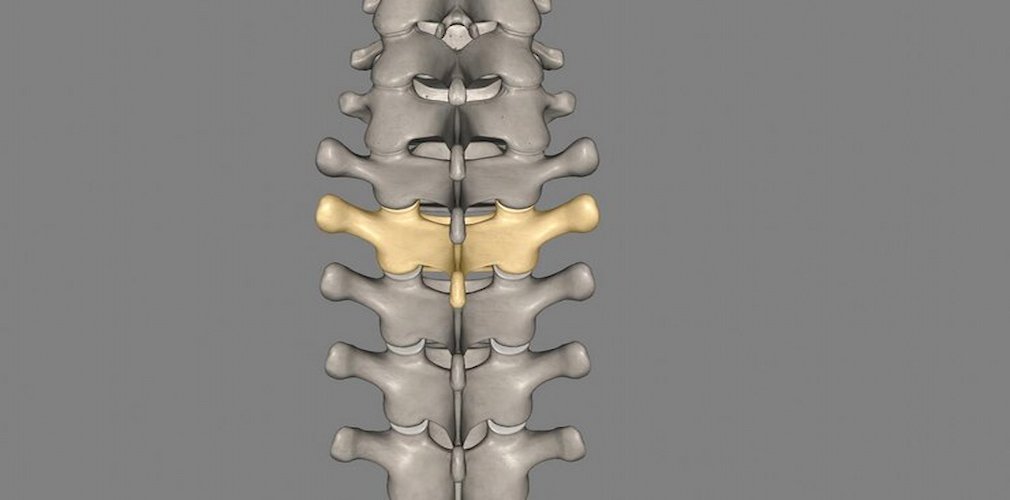
The sciatic nerve is the longest and thickest of the anatomy and is the extension of the fourth, fifth, fifth, first, second and third sacral roots, whose entanglement forms the sacral plexus. Sciatica affects many people. The most important symptoms are pain radiating to the leg and functional problems. Patients are usually treated in primary care but a small proportion are referred to specialists when the problem does not settle and eventually, they are operated.
Diagnosis
An MRI scan is the most definitive method of diagnosing a disc herniation, spinal stenosis or other cause of sciatica.
Approximately 90% of cases are caused by a herniated disc with root compression but stenosis and, less frequently, tumors are also possible causes.
Low back pain is strongly related to disc degeneration, but disc degeneration is also associated with referred pain or “sciatica” and herniated or disc prolapse, which has adverse effects on other vertebral structures such as muscles and ligaments.
Sciatica is diagnosed mainly by assessing symptoms and physical examination. In general, patients report a pain radiating to the leg. In the presentation, doctors can try to identify the distribution of pain and if it radiates below the knee.
Sciatica in Pregnancy
Many factors are responsible for the onset of sciatica in pregnancy, such as weight gain and postural changes throughout this stage.
Pregnancy itself does not cause sciatica, but rather it is a condition that appears in patients who previously had a back injury.
Treatment Plan
- The patient needs to take some rest, but it must not last more than 2 days.
- After a couple of days, it is important to leave the bed and perform a light but progressive physical activity, as you are having less pain.
- The application of local heat many times a day is helpful. Also, a massage when muscles in that area are contracted is especially efficient.
- Take analgesics to relieve pain, such as nonsteroidal anti-inflammatory drugs.
- The regular practice of rehabilitation exercises and sports help in the treatment.
- Sciatic stretches help to keep the nerve moving and should be performed gently.
Prognosis
In general, the clinical course of acute sciatica is favorable and pain and functional impotence resolve within a few weeks. The prognosis is good in most patients, but at the same time, there is a significant proportion (30%) that continues with pain for 1 year or more.
What is the effectiveness of conservative treatments?
The main objective of conservative treatment is to calm the pain, either by means of analgesics or by reducing the pressure on the nerve root. Conservative treatments do not completely improve the natural course of sciatica in most patients or completely reduce their symptoms.
A small difference was found between the effect of bed rest and that of the continuation of activity on pain and functional status. As a result of this finding, bed rest is less recommended-which was, for a long time, the treatment of sciatica.
What is the importance of surgery in sciatica?
The objective of the surgical intervention is to eliminate the herniated disc and eventually the partial removal of the disc or stenosis of the foramen, in order to eliminate the cause of sciatica.
Laser Disc Surgery is a new technique which can be used to treat lumbar disc prolapse without the need for open surgery. A laser probe is used to shrink the disc prolapse.
Frequently Asked Questions
The fastest way to alleviate sciatica symptoms involves a combination of treatments such as rest, anti-inflammatory medications, gentle stretching, and targeted exercises to relieve pressure on the sciatic nerve, along with physical therapy for long-term management.
Avoid activities that exacerbate sciatica symptoms, such as heavy lifting, prolonged sitting, or sudden movements that strain the lower back, and consult a healthcare professional for proper management and treatment.
Yes, walking is generally beneficial for relieving sciatica pain as it helps to stretch and strengthen the muscles supporting the spine while improving circulation, but it’s important to avoid overexertion and consult with a healthcare provider for personalised recommendations.