Home » Archives for THS Hospital » Page 4
Home » Archives for THS Hospital » Page 4
Cervical Disc Replacement
C
ervical disc replacement is a minimally invasive thechnique to remove a degenerate disc and replace it with a moving prosthesis. The procedure can be performed as a day case procedure by our top spinal specialists.
Movement in the Cervical Spine helps to avoid adjacent-level disc degeneration
The cervical disc´s function is to absorb the loads to which the spine is subjected and to cushion the movements that occur between two contiguous vertebrae.
Regarding the factors that influence the appearance of a cervical hernia, we must differentiate between the acute-soft disc hernia that usually occurs in young patients and whose cause is usually traumatic, and the degenerative disc disease, in which the disk appears disc degenerated and dehydrated, and that is typical of cervical osteoarthritis.
The symptoms are of three types: cervical pain, pain referring to the extremities and spinal cord compression.
The diagnostic studies include first the radiography, an electromyogram (EMG), and finally a Nuclear Magnetic Resonance (NMR), which shows the condition of the discs.
What is cervical disc hernia surgery?
It is fundamentally based on removing the entire disc and replace it by a prosthesis. The approach is usually through the anterior aspect of the neck, separating all the prevertebral structures (carotid and esophagus). With microsurgery the disc is removed, the bone peaks are milled and the nerve or marrow is released. There are different techniques but all are based on removing the disc and replacing it with a prosthesis. Cervical hernia surgery performed by highly trained spine surgeons and is quite safe. If a single disc is operated, the surgery usually lasts 45 to 60 minutes, the next day the patient begins to be incorporated and is discharged on the same day or day after. Recovery is usually very fast and the scar heals satisfactorily.
Cervical disc replacement devices
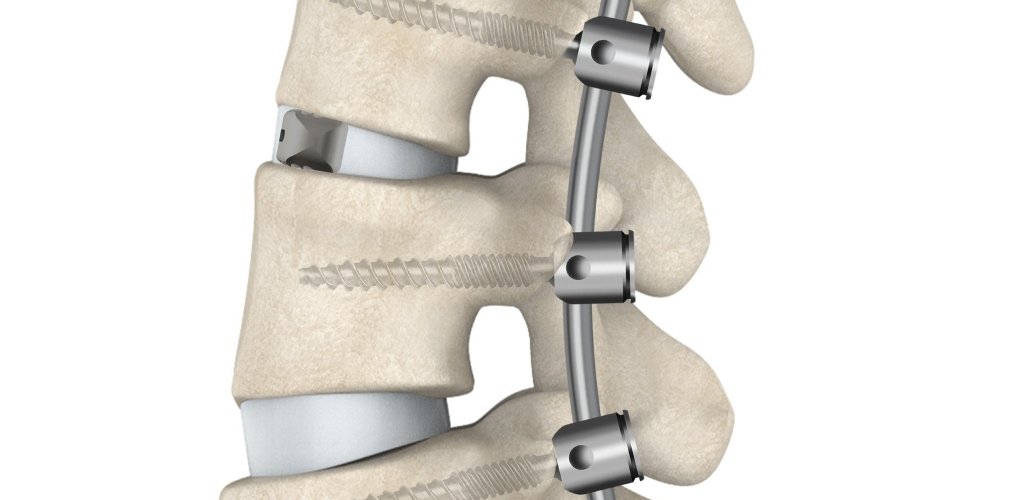
Everything depends on the origin of the hernia: the mobile prosthesis is usually used in soft hernia in young patients without associated degenerative changes. On the other hand, the rigid prostheses are for the other cases or when there is medullar compression, in which it is sometimes necessary to remove one or more vertebrae or to place a plate with screws to favor the stabilization of the spine.
Cervical disc replacement vs. fusion
Recently, fusions have been performed to replace the intervertebral disc, which serves as a buffer between two vertebrae. However, the fusion technique involves adjacent disc degeneration, as a consequence of the increase in the workload suffered by the vertebra situated next to the fused one.
Increasingly, it seeks to preserve as much movement as possible in the spine through the use of prostheses in the intervertebral discs. Prosthetic replacement of the intervertebral disc is a booming technique, which has proven its effectiveness in the short and medium term.
Cervical disc replacement cost
Studies have shown that patients who underwent artificial disc surgery (arthroplasty) have been able to save an average of £4000 in the two years after surgery.
The initial cost of surgery, secondary procedures and medical devices per patient, as well as the cost of the initial procedure, were higher for arthroplasty patients than for fusion patients; however, those who received the artificial disc obtained long-term savings, because they needed fewer secondary procedures and returned to work sooner after surgery than the fusion patients.
Frequently Asked Questions
Cervical disc replacement surgery is generally considered safe and effective, but like any surgical procedure, it carries potential risks, including infection, nerve injury, or complications related to anaesthesia.
Cervical disc replacement surgery has been shown to provide long-term relief from symptoms, with studies indicating that the artificial discs can last for at least 10 to 15 years or more.
Cervical disc replacement surgery has shown high success rates in appropriately selected patients, with many experiencing significant improvement in symptoms and functionality.