Home » Archives for THS Hospital » Page 7
Home » Archives for THS Hospital » Page 7
Posterior Cervical Spine Surgery
C
Cervical Spine Surgery may be indicated for patients with trauma, degeneration, persistent neck pain, and unstable conditions. Surgery to the cervical spine should be undertaken by specialists with experience.
Specialists in Cervical Spine Surgery
Many neck problems are due to degenerative changes that occur in the intervertebral discs of the cervical spine and the joints between each vertebra. Other problems are the result of injury to parts of the spine or complications of earlier surgeries. The vast majority of patients who have neck problems will not require any type of operation. However, if the non-operative treatments fail to control your pain or problems, your spine surgeon may suggest a posterior cervical fusion to treat your neck problem.
The purpose of this information is to help you understand:
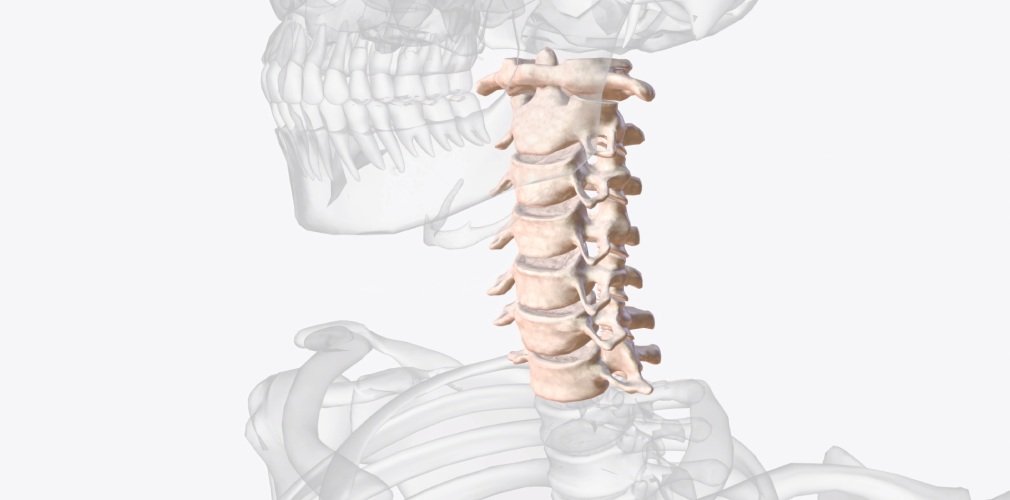
The anatomy of the cervical spine
- The types of problems a posterior cervical fusion is used for
- The rationale for performing a posterior cervical fusion
- What you can expect from this procedure
Anatomy
In order to understand your symptoms and treatment options, you should start with some understanding of the general anatomy of your neck. This includes becoming familiar with the various parts that make up the neck and how these parts work together.
Surgery is not necessary in every case. No one type of surgery works for every neck pain problem. Numerous surgical procedures have been designed to treat each type of neck pain.
A posterior cervical fusion may be recommended for several reasons:
- To stop the motion between two or more vertebrae – or spinal segments
- To straighten the cervical spine and stop the progression of a spinal deformity
- To stabilize the spine after a fracture or dislocation of the cervical spine
The goal of a posterior spinal fusion is to allow two or more vertebrae to grow together or fuse into one solid bone. If the operation is being done because you are suffering from mechanical neck pain, the fusion can stop the excess motion between the vertebrae caused by segmental instability. This can reduce your pain.
If your spine is unstable, due to a fracture or a dislocation of the vertebrae, the fusion stabilizes the spine. This is particularly important when you have not injured your spinal cord. Stabilizing the spine surgically can protect you from spinal cord injury during the healing process. Even in cases when there has been severe damage to the spinal cord leading to paralysis, a spinal fusion may be recommended, so that you can get out of bed and into a wheelchair faster. This allows early rehabilitation because the spine has been stabilized by the internal fixation.
A posterior cervical fusion may also be suggested to straighten the spine, or control a deformity of the cervical spine such as a cervical kyphosis. The cervical spine normally has a “C” shaped curve with the opening towards the back. A “kyphotic” curve is exactly the opposite – the opening of the “C” points forward. This deformity occurs when the cervical spine is unstable and begins to bend forward.
The Operation
Posterior Cervical Fusion
The bone graft is usually taken from the pelvis at the time of surgery, but some surgeons prefer to use bone graft obtained from a bone bank. Bone graft from a bone bank is taken from organ donors and stored under sterile conditions until needed for operations such as spinal fusion. The bone goes through a rigorous testing procedure, similar to a blood transfusion. This is in order to reduce the risk of passing on diseases, such as AIDS or hepatitis, to the recipient.
There are two basic types of cervical spinal fusion:
Anterior Interbody Fusion
This type of fusion is much more common in the neck. This type of fusion is described above. In the interbody fusion, a bone graft is placed between two vertebrae and replaces the removed disc. During the healing process, the vertebrae grow together, creating a solid piece of bone out of the two vertebrae.
Posterior Fusion
In the posterior fusion, the bone graft is placed on the backside of the vertebrae. During the healing process, the vertebrae grow together, creating a solid piece of bone out of the two vertebrae. This type of fusion is used in the cervical spine for fractures and dislocations of the cervical spine, and to correct deformities in the neck such as cervical kyphosis.
Instrumented Posterior Cervical Fusion
When doing an anterior cervical fusion, the bone graft may simply be wedged in between the vertebra. It is held there simply because it is wedged in tight. In the case of a posterior cervical spine fusion, there is not anywhere to wedge bone graft material, so the bone graft is simply laid on top of the lamina of the vertebrae.
In recent years, there has been an increase in the use of metal plates, screws, and rods to try to increase the success of helping the spine to fuse. Many different types of metal implants are used; all try to hold the vertebrae in position while the fusion heals. Bone heals best when it is held still, without motion between the pieces trying to heal together. The healing of a fusion is no different than healing a fractured bone, such as a broken arm. However, the neck is a difficult part of the body to hold still.
In the past, casts and braces were used in an attempt to reduce the motion in the neck and to increase the success rates of a spinal fusion. In most cases, these braces and casts were simply too cumbersome to wear for three months, and did a poor job of actually holding the neck still enough to allow the fusion to heal.
In the posterior cervical spine fusion, it is common to use stainless steel wire to hold the bones together as they heal. The wires are wrapped around the spinous processes, or under the lamina and twisted together. This creates a fairly strong form of internal fixation that holds the bones in place while they heal.
By using wires, the vertebra can be held rigidly in place while the fusion heals. Braces and casts are not needed.
Complications
With any surgery, there is a risk of complications. When surgery is done near the spine and spinal cord these complications (if they occur) can be very serious. Complications could involve subsequent pain and impairment and the need for additional surgery. You should discuss the complications associated with surgery with your doctor before surgery. The list of complications provided here is not intended to be a complete list of complications and is not a substitute for discussing the risks of surgery with your doctor. Only your doctor can evaluate your condition and inform you of the risks of any medical treatment he or she may recommend.
Frequently Asked Questions
Posterior cervical spine surgery is a surgical procedure performed on the back of the neck to address conditions affecting the cervical spine, such as herniated discs, spinal stenosis, or degenerative disc disease. It involves accessing the spine through the back of the neck to relieve pressure on the spinal cord or nerves and stabilise the affected area.
Common reasons for posterior cervical spine surgery include severe neck pain, weakness, or numbness in the arms, difficulty walking, or loss of bladder or bowel control due to compression of the spinal cord or nerves. Surgery may be recommended when conservative treatments such as medication, physical therapy, or injections fail to provide adequate relief.
Recovery from posterior cervical spine surgery varies depending on the specific procedure performed and individual factors. It typically involves a hospital stay of a few days, followed by a period of restricted activity and physical therapy to regain strength and mobility. Pain management and adherence to post-operative instructions are essential for optimising recovery and achieving the best possible outcome.