Home » Archives for THS Hospital » Page 13
Home » Archives for THS Hospital » Page 13
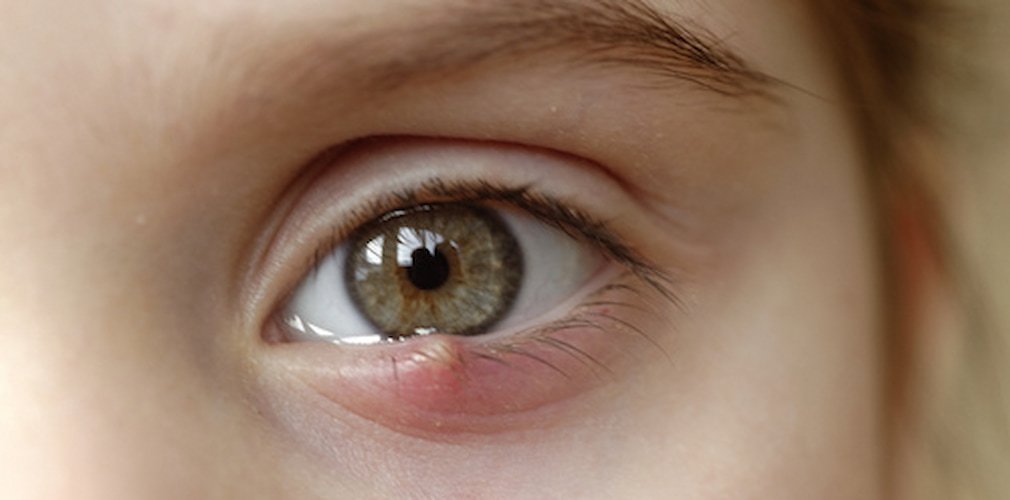
Discharge from Eyes
O
cular secretion is a fluid composed of mucus, oil, skin cells and other waste accumulated in the inner corner of the eye. Normally this secretion occurs while we sleep and can be wet or dry, depending on the level of fluid contained.
The ocular secretion corresponds to one of the many ways in which the body protects our eyes. This since said mucus removes potentially damaging waste and sediments from the tear film.
The presence of a mild ocular discharge upon awakening is normal, however, excessive secretion could indicate the presence of an infection or condition in the eyes. It is important to pay attention to the color of the secretion, since, if it has a green or yellow color and is accompanied by blurred vision, light sensitivity or eye pain, it should be examined by an ophthalmologist as soon as possible.
Symptoms of excessive ocular discharge:
- Yellowish or greenish secretion of pus in one or both eyes.
- The eyelids are stuck with pus after sleeping.
- The pus comes back during the day after having cleaned it.
The causes of ocular secretion may include:
- Allergies, including seasonal or allergic rhinitis.
- Bacterial or viral infections (conjunctivitis).
- Chemical irritants (such as chlorine in a pool or makeup).
- Irritants in the air (cigarette smoke or smog).
- Inflammatory conjunctivitis (red eye).
- Obstruction of the tear duct.
- Dry eye.
- Ulcers of the cornea (keratitis).
It is recommended that in the presence of any of the symptoms of an abnormal ocular discharge detailed throughout this article, immediately attend a specialized center such as Harley Street Hospital, for the early detection and appropriate treatment of the pathology.
Frequently Asked Questions
Mucus discharge from the eye can indicate irritation, infection, or an underlying condition such as conjunctivitis or dry eye syndrome, and it’s best to consult with an eye doctor for proper diagnosis and treatment.
Eye discharge can be due to various reasons, including allergies, infections (such as conjunctivitis), dry eyes, or environmental irritants, and consulting with an eye care professional is recommended for proper diagnosis and treatment.
Eye mucus can be treated by gently cleaning the eyes with a warm, damp cloth and using artificial tears or saline solution to help soothe irritation and remove excess mucus. If the problem persists or is accompanied by other symptoms, it’s important to consult an eye care professional for further evaluation and treatment.